Papua New Guinea is battling the world's oldest pandemic: malaria. How can it get back on track?
来源:World Economic Forum;发表于:2022-02-17;人气指数:535
Papua New
Guinea is battling the world's oldest pandemic: malaria.
How can it get back on
track?
https://www.weforum.org/agenda/2021/09/papua-new-guinea-malaria/
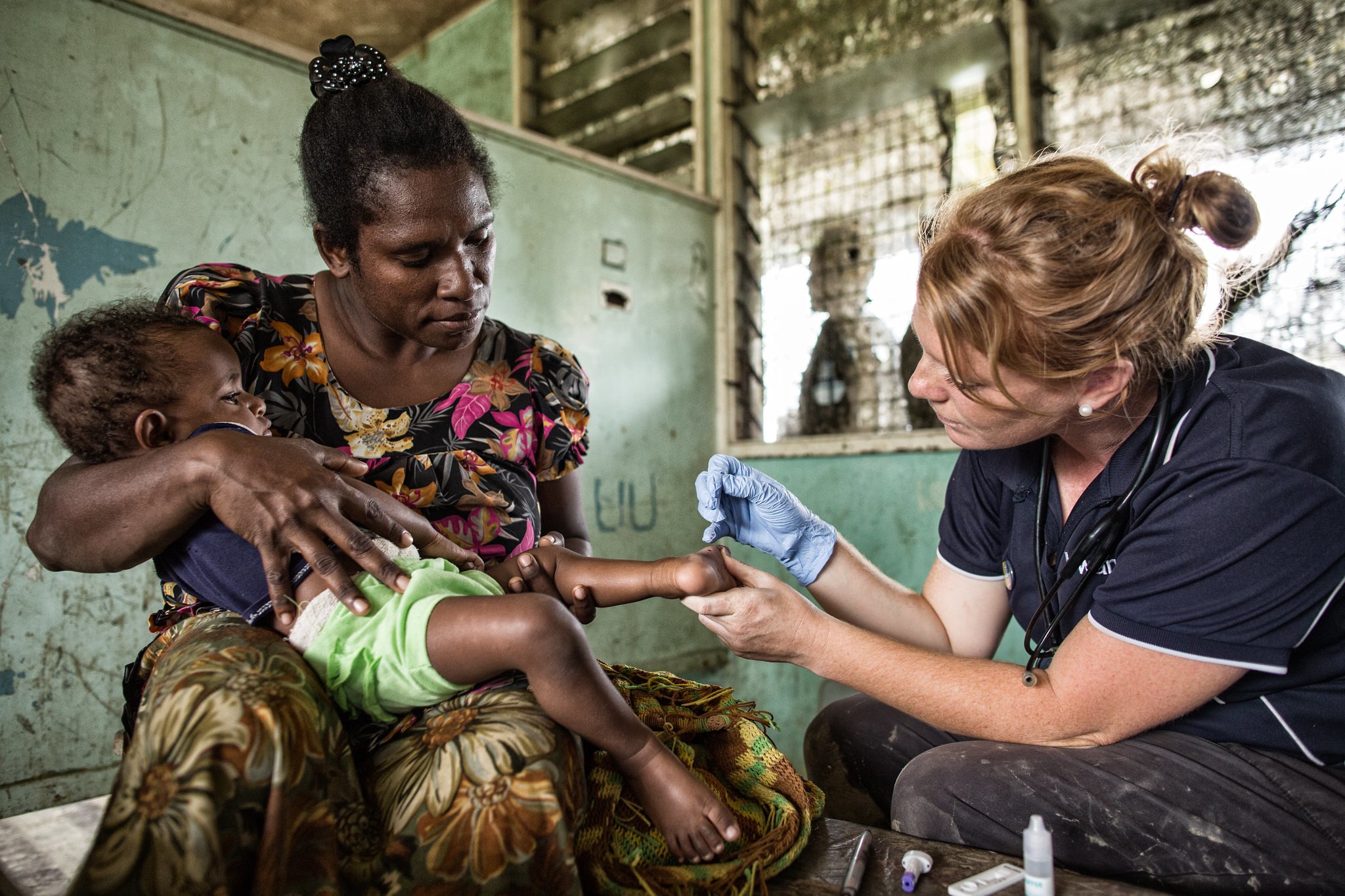
A medical worker
conducts a precautionary malaria test at a health centre in Baimuru, Papua New
Guinea.
Image: YWAM
13 Sep 2021
Sarthak Das
CEO, Communicable
Disease Threats Initiative & Asia Pacific Leaders Malaria Alliance
*Malaria cases in
Papua New Guinea have increased more than tenfold in five years.
*The country's
progress on TB and HIV despite its limited resources provides reasons for
optimism.
*Infrastructure,
funding and leadership structures are paramount for eliminating malaria.
With only 1% of the
world’s land mass and a population of under 9 million, Papua New Guinea (PNG)
is one of the most biologically and culturally diverse places on earth, and
home to over 850 active languages. Unfortunately, there are also severe
limitations in resources for health delivery, with barely one doctor per
10,000 people (the United States has about three per 1,000); its
incredibly rugged terrain has posed continual challenges for economic and
social development more broadly (PNG ranks 155th out of 189 on
the United Nation’s Human Development Index). PNG also has the highest
malaria burden in the Asia Pacific region – it accounted for nearly a
third of cases in 2019. But this was not always the case.
The country had seen
a steady decline in malaria cases leading up to 2014, but as data illustrates,
this changed rapidly in the span of only five years. In fact, cases increased
over tenfold from 50,309 in 2014 to 646,648 in 2019. This
alarming resurgence has been attributed to a variety of factors, from
reduced government and donor commitment, limited access to key treatment and
diagnostic tests, reduced effectiveness of long-lasting insecticidal nets
(LLINs), to the challenges of a fully devolved health system. Encouragingly,
however, an investment case developed by the University of California
San Francisco (UCSF) revealed not only an estimated return of 9:1 on investment
in malaria elimination, but also that elimination is technically feasible.
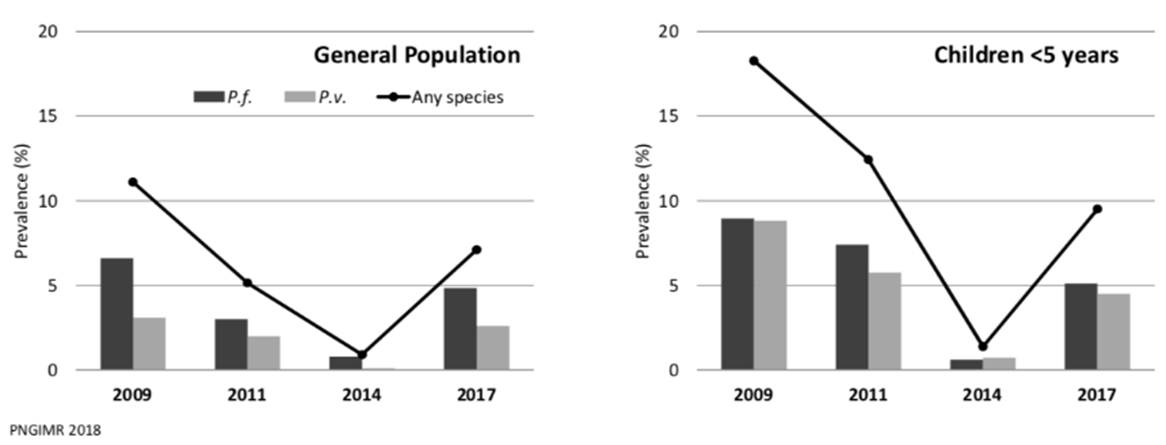
Prevalence of malaria
in Papua New Guinea.
In fact, PNG’s
promising progress in managing two other infectious diseases, HIV and
tuberculosis (TB), despite limited resources is worth noting. Targeted focus on
expanding coverage of antiretroviral therapy (ART) from an estimated 23 to 65%
from 2010 to 2020 has resulted in a significant drop in deaths, as has
prioritizing TB/HIV linkages in high TB burden provinces.
Despite a myriad of
challenges, PNG has successfully built systems addressing complex conditions:
whether for chronic disease, in the case of HIV, or in battling acute
HIV-associated or multi-drug resistant TB (MDR-TB). In June this year, PNG
successfully transitioned out of the World Health Organization (WHO)’s global
list of high burden countries for HIV-associated TB.
Building on these
successes and getting the country back on track for malaria elimination is
critical and will help to save both money and precious resources for the
country as it tackles the ongoing COVID-19 pandemic alongside other high-burden
diseases.
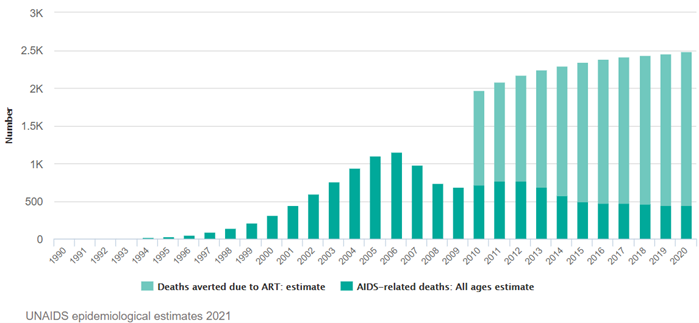
Number of
AIDS-related deaths vs. number of deaths averted due to ART.
Image: UNAIDS
There are three key
things we can do to help bring PNG back on track with regard to malaria:
First, disease-dedicated
investment must be linked to infrastructure that meaningfully improves
public health. This can be achieved by ensuring governments, foundations and
funders support better coordination of health and infrastructure investments in
PNG. The country has one the lowest provisions of safe water supply in
the world and only an estimated eighth of the population has access to grid-connected
electricity. This means that PNG needs power and clean water as much as
sophisticated diagnostics or pharmaceuticals.
Take for example
vaccine distribution efforts under the COVID-19 Vaccines Global Access (COVAX)
facility: Despite the facility securing up to 40 million doses of
Pfizer-BioNTech’s cutting-edge vaccine early on, its infrastructure demands,
including the need for ultra-low temperature storage, meant PNG could not
even realistically receive or dispatch them.
Second, while surging
investments in ending malaria are indeed the pathway to eradication and will
strengthen PNG's ability to respond to future threats, funding needs to
last long enough to do the job. Pouring money into health systems for two
or three years as is often the case is insufficient; it takes at least four to
five years – with rigorous milestones for progress – to achieve lasting
results.
External technical
support needs time to earn local trust. Stretching health projects over longer
periods and requiring that they involve a greater proportion of local
personnel, especially given PNG’s chronic shortage of skilled human
capital in the heath sector, will better ensure sustainable results.
Funding for local projects should therefore include specific targets for local
participation, with a key metric being that of public sector “absorption” of
staff into national or sub-national programs.
Finally, there is a
need for strong leadership and sustained political will at multiple
levels – not solely at the national level, but also at the sub-national
and community levels. This is especially true in the case of PNG where the
health sector has seen several decentralization efforts since
independence, such that Provincial Health Authorities (PHAs) and District Development
Authorities (DDAs) have significant budgetary autonomy at the sub-national
level. To effectively translate political will into action and impact,
sub-national leadership at the district, provincial and state levels is
critical. Strong local leadership can support sub-national tailoring of
interventions based on locally available data to maximize impact. Joining the
dots coherently between all levels of governments, from heads of state right to
the hearts of communities, including the most vulnerable and hard to reach, will
be key to driving an effective malaria response.
As the Global
Fund's 2021 Results Report highlighted, COVID-19 has been the most
significant setback in the fight against HIV, TB and malaria in two decades –
key programmatic results across these three diseases declined, putting already
vulnerable populations further at risk. The pandemic’s silver lining is that it
has given global leaders and health policy-makers an extraordinary opportunity
to build durable systems instead of applying band-aids.
There has never been
a more urgent time to ensure that we invest in the right infrastructure, for long
enough and with the right people involved. Only then might we be able to put an
end to the over 400,000 preventable malaria deaths annually, and to manage what
continues to be the world’s longest-running pandemic.